Case Challenge
By Brad Gettleman, D.D.S., M.S.
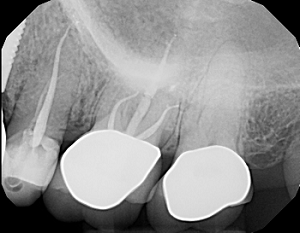
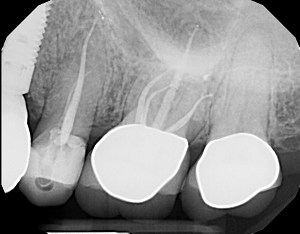
A 40-year-old Caucasian female had non-surgical endodontic therapy completed approximately two months prior. The patient was ASA 1 with a non contributory health history.
The patient's original symptoms were severe thermal sensitivity and mild chewing discomfort. The pre-operative diagnosis was irreversible pulpitis with symptomatic apical periodontitis. Patient reports that the nature of the pain has changed, but has not resolved, since the treatment was completed. Following treatment, she has periodic heat sensitivity and the chewing discomfort has worsened. Radiographic assessment (PA and CBCT) revealed a missed MB2. Heat sensitivity could not be reproduced; however, the tooth responded severely to percussion. The occlusion was not an issue.
The post-operative diagnosis was previous endodontic therapy with symptomatic apical periodontitis.
Selective retreatment, or treatment of the missed MB2, was performed and the symptoms resolved. The concept of only treating the diseased root will need further investigation; however, this is mentioned in recent literature. This is very much the way practitioners have approached surgical endodontic cases for decades.
Vitals:
Blood Pressure: 123/83
Heart Rate: 70
Was selective retreatment the best treatment option or should the entire case have been retreated? Any liability concerns? Select a treatment option below. We'll provide the best answer in a future edition of The Paper Point.
Dr. Brad Gettleman is board liaison for the AAE’s Resident and New Practitioner Committee.