Case Challenge: August 2018
By Mary Um, D.M.D.
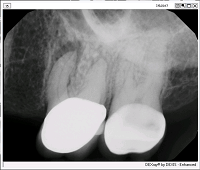
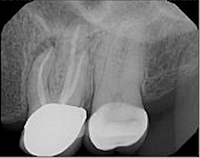
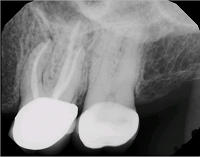
A 65-year-old white female presented for six-month follow-up after non-surgical root canal treatment on #14 completed by an endodontic resident. The patient reported unremitting pain (8/10) that occasionally worsens of its own accord. She also noted localized swelling of the gingival tissue and pain with flossing around tooth #14 several times in the last three months.
Med Hx: ASA II: hypothyroidism and fibromyalgia. She reports last flare-up six years ago. Review of systems was otherwise unremarkable.
Surgical Hx: Appendectomy (1962), C-Section (1976), Tubal ligation (1982), Tonsillectomy (1992), Hysterectomy (2000), Cholecystectomy (2002).
RX: Synthroid 175mcg 1/day.
Allergies: Bextra/Valdecxib, Celebrex, Darvaset, Demeral, Singulair, Sulfa.
Hx Current Illness: #14 RCT was completed 6 month ago. Pre-op diagnosis was pulpal necrosis and symptomatic apical periodontitis. She had initially presented with mild intraoral swelling, which resolved after treatment. Patient reports that the nature of pain has changed since the root canal has been completed but has not resolved. Now, the pain has a radiating and pulsating quality.
Radiographic assessment is suggestive of a 1-mm overextension of obturation material. A post-operative CBCT scan suggests that no separate MB2 canal is present. Post-operative imaging is suggestive of periapical bony healing around MB root of #14. However, the buccal plate remains perforated. No sinus membrane inflammation noted. Remainder of CBCT scan is unremarkable.
| 12 | 14 | 15 | |
|---|---|---|---|
| Cold | + | - | + |
| Palp | - | + | - |
| Perc | - | + | - |
Probing depth: 3-4mm circumferentially.
In the December 2017 Case Challenge, we posted a poll; and now have the results below:
| A soft tissue biopsy of the lesion in the area of #7 was obtained. Given the historical, clinical, and radiographic findings of this case, which of the following diagnoses on the differential is most likely to reflect the patient’s condition? |
|---|
The Best Answer is B.