Root Canal Explained
Has your dentist or endodontist told you that you need root canal? If so, you're not alone. More than 15 million teeth are treated and saved each year with the root canal, or endodontic, treatment. This page explains root canal treatment in detail and how it can relieve your tooth pain and save your smile.
 “Endo” is the Greek word for “inside” and “odont” is Greek for “tooth.” Endodontic treatment treats the inside of the tooth. Root canal treatment is one type of endodontic treatment.
“Endo” is the Greek word for “inside” and “odont” is Greek for “tooth.” Endodontic treatment treats the inside of the tooth. Root canal treatment is one type of endodontic treatment.
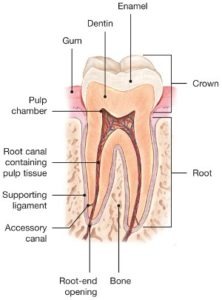
To understand endodontic treatment, it helps to know something about the anatomy of the tooth. Inside the tooth, under the white enamel and a hard layer called the dentin, is a soft tissue called the pulp. The pulp contains blood vessels, nerves and connective tissue and creates the surrounding hard tissues of the tooth during development.
The pulp extends from the crown of the tooth to the tip of the roots where it connects to the tissues surrounding the root. The pulp is important during a tooth’s growth and development. However, once a tooth is fully mature it can survive without the pulp, because the tooth continues to be nourished by the tissues surrounding it. Learn more about exactly what a root canal is.
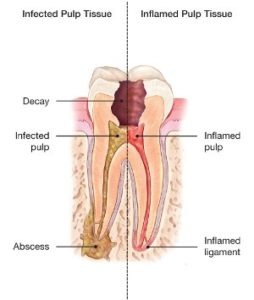
Endodontic treatment is necessary when the pulp, the soft tissue inside the root canal, becomes inflamed or infected. The inflammation or infection can have a variety of causes: deep decay repeated dental procedures on the tooth or a crack or chip in the tooth. In addition, an injury to a tooth may cause pulp damage even if the tooth has no visible chips or cracks. If pulp inflammation or infection is left untreated, it can cause pain or lead to an abscess.
There are a few symptoms that mean you might need a root canal—
- Severe pain while chewing or biting
- Pimples on the gums
- A chipped or cracked tooth
- Lingering sensitivity to hot or cold, even after the sensation has been removed
- Swollen or tender gums
- Deep decay or darkening of the gums
The endodontist removes the inflamed or infected pulp, carefully cleans and shapes the inside of the root canal, then fills and seals the space. Afterward, you will return to your dentist, who will place a crown or other restoration on the tooth to protect and restore it to full function. After restoration, the tooth continues to function like any other tooth.
Many endodontic procedures are performed to relieve the pain of toothaches caused by pulp inflammation or infection. With modern techniques and anesthetics, most patients report that they are comfortable during the procedure.
For the first few days after treatment, your tooth may feel sensitive, especially if there was pain or infection before the procedure. This discomfort can be relieved with over-the-counter or prescription medications. Follow your endodontist’s instructions carefully.
Your tooth may continue to feel slightly different from your other teeth for some time after your endodontic treatment is completed. However, if you have severe pain or pressure or pain that lasts more than a few days, call your endodontist.
 Endodontic treatment can often be performed in one or two visits and involves the following steps:
Endodontic treatment can often be performed in one or two visits and involves the following steps:
- The endodontist examines and takes a radiograph of the tooth using x-rays, then administers local anesthetic. After the tooth is numb, the endodontist places a small protective sheet called a “dental dam” over the area to isolate the tooth and keep it clean and free of saliva during the procedure.
- The endodontist makes an opening in the crown of the tooth. Very small instruments are used to clean the pulp from the pulp
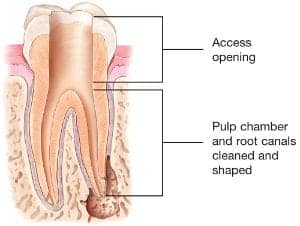 chamber and root canals and to shape the space for filling.
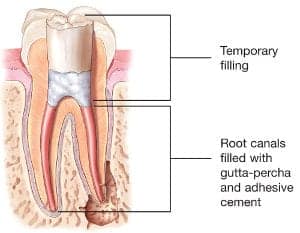
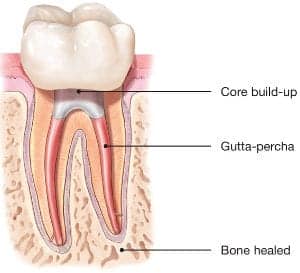
chamber and root canals and to shape the space for filling. - After space is cleaned and shaped, the endodontist fills the root canals with a biocompatible material, usually a rubber-like material called gutta-percha. The gutta-percha is placed with an adhesive cement to ensure complete sealing of the root canals. In most cases, a temporary filling is placed to close the opening. The temporary filling will be removed by your dentist before the tooth is restored.
- After the final visit with your endodontist, you must return to your dentist to have a crown or other restoration placed on the tooth to protect and restore it to full function.
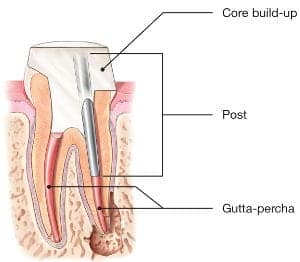
If the tooth lacks sufficient structure to hold the restoration in place, your dentist or endodontist may place a post inside the tooth. Ask your dentist or endodontist for more details about the specific restoration planned for your tooth.
The cost varies depending on how complex the problem is and which tooth is affected. Molars are more difficult to treat; the fee is usually more. Most dental insurance policies provide some coverage for endodontic treatment.
Generally, endodontic treatment and restoration of the natural tooth are less expensive than the alternative of having the tooth extracted. An extracted tooth must be replaced with an implant or bridge to restore chewing function and prevent adjacent teeth from shifting. These procedures tend to cost more than endodontic treatment and appropriate restoration.
You should not chew or bite on the treated tooth until you have had it restored by your dentist. The unrestored tooth is susceptible to fracture, so you should see your dentist for a full restoration as soon as possible. Otherwise, you need only practice good oral hygiene, including brushing, flossing, and regular checkups and cleanings.
Most endodontically treated teeth last as long as other natural teeth. In a few cases, a tooth that has undergone endodontic treatment does not heal or the pain continues. Occasionally, the tooth may become painful or diseased months or even years after successful treatment. Often when this occurs, redoing the endodontic procedure can save the tooth.
New trauma, deep decay, or a loose, cracked or broken filling can cause new infection in your tooth. In some cases, the endodontist may discover additional very narrow or curved canals that could not be treated during the initial procedure.
Most teeth can be treated. Occasionally, a tooth can’t be saved because the root canals are not accessible, the root is severely fractured, the tooth doesn’t have adequate bone support, or the tooth cannot be restored. However, advances in endodontics are making it possible to save teeth that even a few years ago would have been lost. When endodontic treatment is not effective, endodontic surgery may be able to save the tooth.
After a root canal, try to eat soft foods that require very little chewing, like applesauce, yogurt, eggs, and fish. Avoid hard or hot foods that might hurt your teeth. Some dentists suggest to not eat for a few hours until the numbness in your mouth wears off so you don’t bite your cheek or tongue.
A root canal is performed when the endodontist removes the infected pulp and nerve in the root of the tooth, cleans and shapes the inside of the root canal, then fills and seals the space. Afterward, your dentist will place a crown on the tooth to protect and restore it to its original function.
For the first few days after a root canal, some patients experience sensitivity, swelling, or inflammation, while others experience an uneven bite or a reaction to the medication provided by the endodontist. Regardless of symptoms, a follow-up appointment is almost always needed.
A root canal does not kill the tooth, and after a root canal is complete, the tooth will be able to function as it normally does. However, root canals do remove the nerves inside the tooth, but these nerves serve very little function in a fully formed tooth.
Needing a crown after a root canal depends highly on the location of the tooth in the mouth—teeth towards the back of the mouth like molars and premolars are needed more for chewing, and generally require crowns, where incisors or canines which aren’t needed for chewing don’t always require crowns.
Root canals can fail for a variety of reasons, including a procedure that didn’t clean the canals to begin with, a breakdown of the crown or its inner sealant, or essentially anything that allows the tooth that previously had a root canal treatment to become infected at the root and affect other teeth.
If left untreated, the infection in the tooth can spread to other parts of the body, and in some cases can even be life threatening. If you are in need of a root canal, the infected pulp in the tooth needs to be removed.
There is absolutely no evidence that a root canal can cause cancer. In fact, a root canal is the only way to remove an infected tooth that could spread and cause serious disease or illness. All claims that root canals cause cancer or other illnesses are complete myths.
Unless told otherwise by your dentist or endodontist, brush and floss as you regularly would after a root canal treatment.
Sometimes after a root canal, the tooth can become slightly discolored or develop spots called intrinsic stains, where the tooth bleeds internally and the inner part of the tooth turns yellow or dark. Luckily, the tooth can be whitened afterward through internal (non-vital) bleaching.
Most root canals can be done in one to two appointments. The first appointment is the procedure itself when the infected pulp is removed. The second (and maybe third) appointment is when the root canal gets cleaned and filled with a crown or other filling to prevent infections. Each appointment lasts roughly 90 minutes each.
While you can smoke after a root canal it is not recommended as smoking increases the risk of needing another procedure. In fact, smokers are nearly twice as likely to need root canals than non-smokers, and that number increases with more years of smoking.
Most root canal procedures are done using local anesthesia, meaning only the areas that are being operated on will be numb during the course of the procedure. This means you are awake and aware during the process and can drive and operate machinery as you normally would immediately after the procedure is over.
While all general dentists have been trained in root canals, more often than not the procedure is done by an endodontist. Generally speaking, a dentist specializes in exterior teeth and gum health, an endodontist specializes in the health of the inside of the tooth.
Waiting too long to get a root canal can oftentimes result in tooth loss. This generally occurs when the root of an infected tooth has gone untreated for so long that results in bone loss. Many times with severe furcation, it might be too late for a root canal and the tooth would need to be extracted.
You can eat normally before a root canal treatment, and most endodontists even allow patients to eat up to 1 hour before a procedure. However, as with all oral procedures, most endodontists prefer that you brush your teeth prior to the appointment.
It is always better to maintain a healthy, natural smile whenever possible, and root canals allow for just that. Extracting and then replacing a tooth results in more treatments and procedures, and could even impact neighboring teeth and supporting gums.
Generally speaking, most endodontists choose local anesthesia for a root canal, meaning they are only numbing the area that needs to be operated upon. However, the option for general anesthesia varies from endodontist to endodontist, and it’s best to consult your local office about their policies.
After a root canal procedure, you can eat and drink normally, including alcohol, once the numbness wears off.
After a root canal, make sure to follow all of your endodontist’s instructions, which most often include avoiding hard or especially chewy foods, brushing twice a day, and being very cautious around the area where the root canal procedure was completed.




