Case Challenge
By Dr. Ron Hill
A 55-year-old Caucasian female was referred for evaluation of tooth #8. She has no chief complaints. On recent examination, a periapical lesion was noted on tooth #8. She gives a history of a fall in second grade that caused her tooth to fracture. She remembers going in several times for “root canal treatment”, but states that they never could “get it to close”. She remembers little else about subsequent treatment.
Her health history is unremarkable with no history of illnesses and no current prescription medications. She reports allergies to sulfa and opioids. She does state that her physician wants her to start taking Fosamax due to age related osteoporosis, and her general dentist would like to know whether treatment needs to be done prior to her starting the medications and whether an implant needs to be considered if endodontic treatment is not-favorable. Her bisphosphonate dosage will be 20 mg orally once weekly.
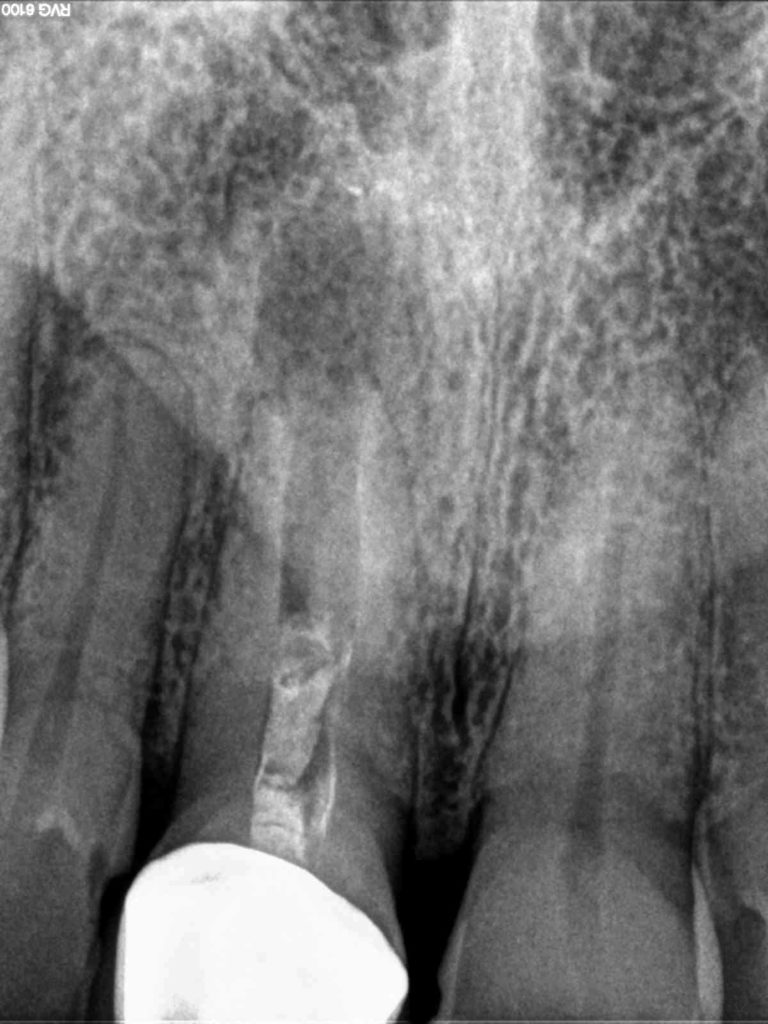
Imaging shows tooth #8 with a blunderbuss apex and a moderate sized periapical lesion. The canal space is filled to the middle-third with an opaque substance that is not dense and is likely calcium hydroxide based on the patient’s history and was probably an attempt at apexification. On clinical exam, there is a PFM crown on the tooth that has been present for many years. Although there is mild recession and the margins are exposed, the marginal integrity is good and there is no caries. Tissue health appears excellent, with probing depths of 1-2 mm and physiologic mobility. There is no swelling or sinus tract in the apical tissues. Diagnostic testing indicates no response to Endo Ice and no pain to bite or percussion.
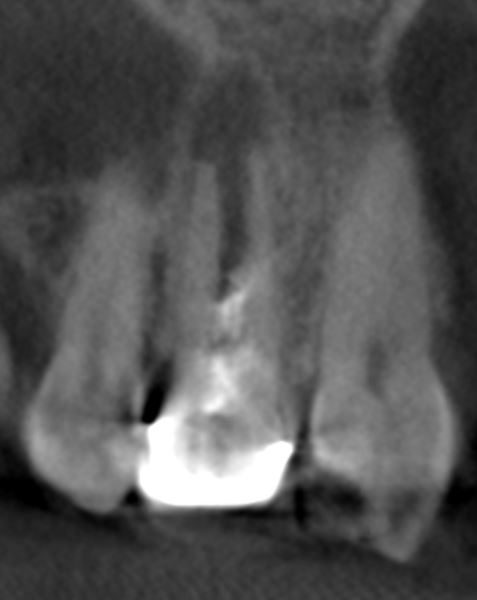
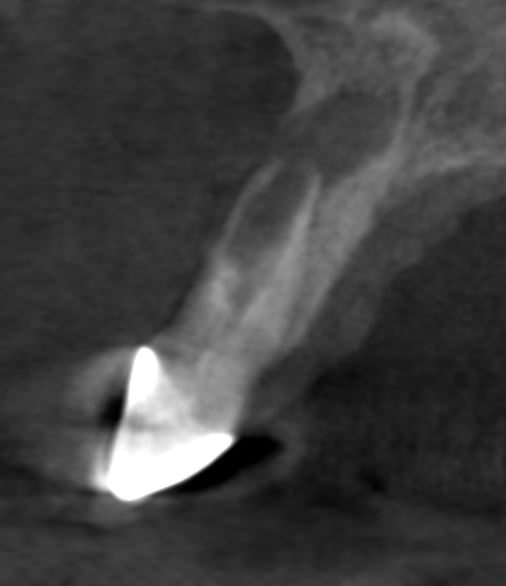
CBCT was done and confirms blunderbuss apex and moderate periapical lesion that has eroded the labial cortical plate despite the lack of swelling or sinus tract.
Dr. Ron Hill is board liaison for the AAE's Resident and New Practitioner Committee. He is also in private practice and is a clinical assistant professor for the Department of Endodontics at the University of Texas School of Dentistry, where he teaches both graduate and undergraduate students.
In the August 2018 Case Challenge, we posted a poll; and now have the results below:
- 12%
- 18%
- 36%
- 18%
- 8%
Best answer: D. Given the context of the patient’s medical history, she was referred to an oral medicine specialist to rule out the potential contribution of a fibromyalgia flare-up. After two months of varying high-dose gabapentin (up to 1200 mg), the patient’s pain level has reportedly dropped from 8/10 to 2/10. She remains under the care of the oral medicine specialist.